The 4 Most Dangerous Myths About Diabetic Foot Wounds
When you are managing diabetes, elevated blood sugar levels can damage delicate nerves (diabetic neuropathy) and restrict blood flow (peripheral artery disease). This means a minor scrape that a healthy person would heal in a week can rapidly escalate into a life-threatening ulcer.
Because the stakes are so high (and because the internet is full of terrible DIY advice), following outdated “home remedies” can lead to catastrophic infections or amputation. We often see patients who have accidentally made their foot wounds worse by following bad advice,” says Dr. Kunal Amin. When it comes to diabetic wound care, doing the ‘wrong’ thing is often much more dangerous than doing nothing at all.
With that in mind, Cypress Foot & Ankle created the following blog. Read on to learn the facts about diabetic foot care, how we actually heal diabetic wounds, and more.
Myth 1: “If my foot doesn’t hurt, the cut isn’t serious.”
The Truth: This is the most dangerous myth of all.
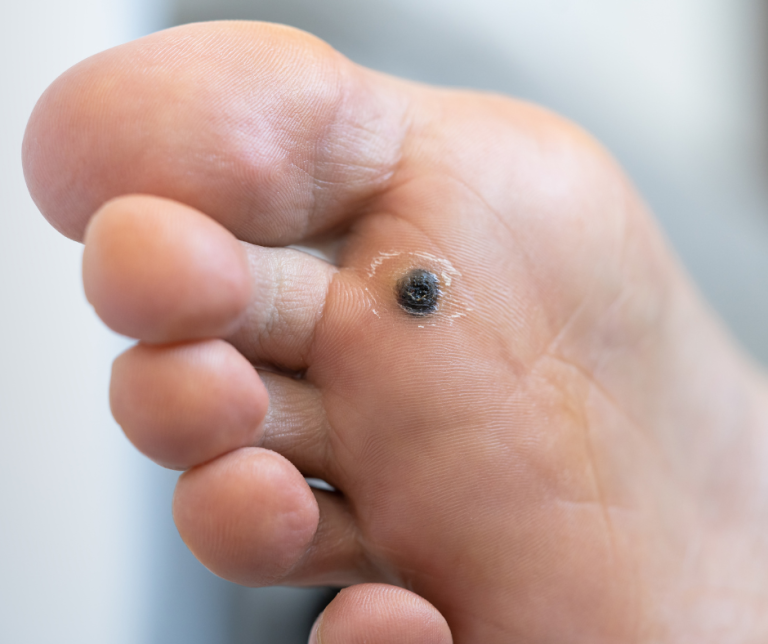
Neuropathy acts like a severed alarm wire. Your foot could be pierced by a nail, severely blistered by a tight shoe, or develop a deep pressure ulcer, and your brain will never receive the “pain” signal.
- You cannot rely on pain to tell you something is wrong. You must rely on your eyes.
- Diabetics must visually inspect the bottoms of their feet every single night (using a hand mirror if necessary) to catch “silent” wounds.
- If you see blood, redness, or swelling, it is a medical emergency…even if your pain level is zero.
Myth 2: “Soaking in hot Epsom salt water will clean the infection.”
The Truth: You should never soak a diabetic foot wound in hot water.
- Because of neuropathy, you cannot accurately gauge temperature. Patients frequently sustain severe, third-degree burns from bathwater because they simply couldn’t feel that the water was scalding.
- Furthermore, soaking macerates (waterlogs) the skin, making it highly susceptible to tearing, and it can actually push surface bacteria deeper into an open wound.
- Wash your feet quickly with lukewarm water and a washcloth, and dry thoroughly between the toes.
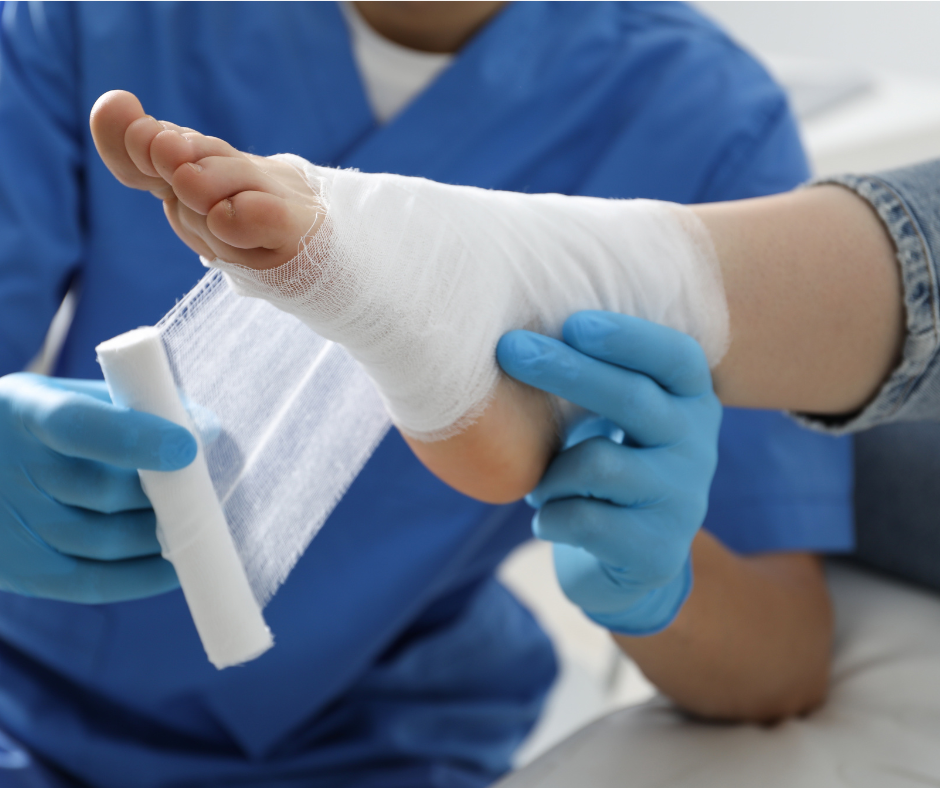
Myth 3: “Leave the wound uncovered to ‘breathe’ and dry out.”
The Truth: A dry wound is a dead wound. The old advice of letting a scrape “air out” and form a hard scab actually slows down cellular repair.
- Medical science shows that wounds heal significantly faster in a clean, moist, and protected environment.
- Leaving a diabetic ulcer exposed to the open air invites bacteria from the floor and your socks directly into your bloodstream.
- Always keep wounds covered with a sterile dressing recommended by your podiatrist.
Myth 4: “I can just use medicated pads from the pharmacy to remove my calluses.”
The Truth: Over-the-counter “corn remover” or callus pads contain harsh chemicals, usually Salicylic Acid.
- Acid does not know the difference between a dead callus and healthy, living tissue.
- For a diabetic with compromised circulation, these pads frequently cause severe chemical burns that quickly turn into gaping, infected ulcers.
- Never use sharp blades, cheese graters, or chemical pads on your feet.
The Fact-Based Fix
A specialist must manage diabetic foot care. Dr. Amin and Dr. Siddiqui specialize in comprehensive diabetic limb salvage and advanced wound care. From prescribing specialized diabetic shoes to offload pressure, to utilizing advanced wound healing protocols, we focus on saving tissue and preventing complications before they start.
Experiencing pain or seeking preventative care? Cypress Foot & Ankle Center offers a wide range of services to address all your foot and ankle needs. While we focus on non-surgical treatments, our team also provides advanced surgical procedures when necessary, using the latest technologies to ensure superior outcomes. Call (281) 377-4040 or contact us online.